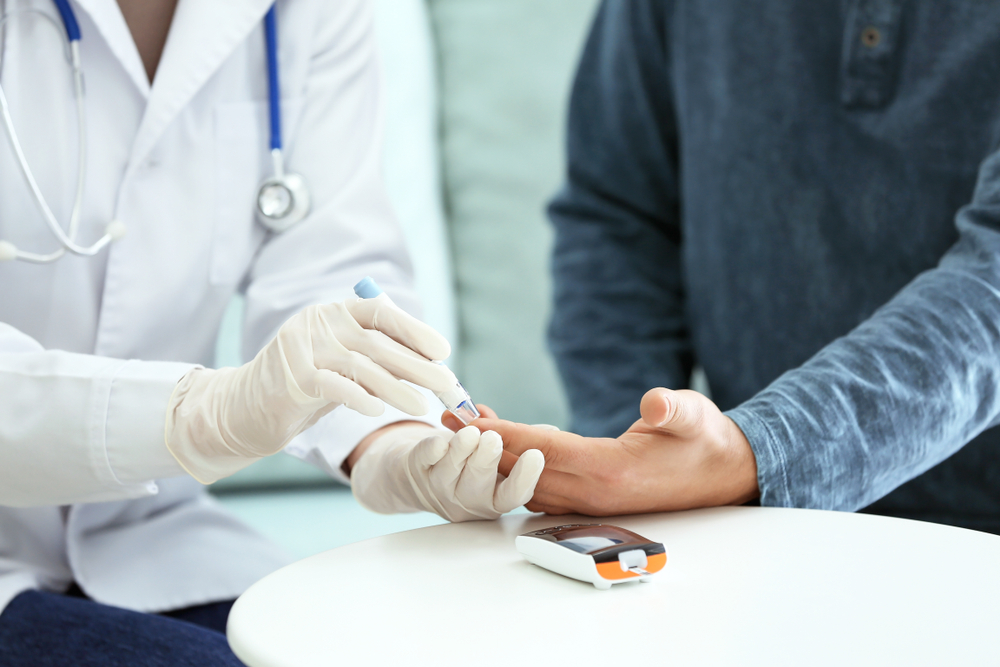
Diabetes and Vein Health: What's the Link?
If you are one of the 30 million Americans currently affected by diabetes, you have to constantly worry about your insulin, blood-glucose levels, diet, your feet, getting an infection, and your circulation. People with diabetes know that it affects their circulation and ability to fight infection. It can even result in their biggest fear: losing their foot or leg and being handicapped. They often tell me the story of a family member with diabetes who lost their leg. They are deathly afraid of this, and they don’t want it to happen to them. So the question is: how is diabetes related to vein conditions? The following is based on my perspective as a cardiovascular surgeon and vein care specialist who regularly sees people with diabetes and circulation problems.
Diabetes and circulation – what are the problems?
- Arterial disease, called PAD (peripheral artery disease): This is often associated with pain with walking and it can lead to limb loss or even a situation requiring emergency surgery. This condition is due to a buildup of blockages in the arteries. The common symptoms are calf pain when walking, sores on the tips of the toes, or non-stop pain in the feet.
- Foot sores and neuropathy: The individual can’t feel their feet and a sore develops on the foot leading to uncontrolled infection. The sores are on the bottom of the toes or feet and are due to loss of protective sensation. Because people can’t feel the sore, they can worsen dramatically. The sore often burrows deep into the bones of the foot which makes healing much more difficult. It can result in toe or foot amputation.
- Cellulitis: This is an infection of the skin of the leg and often occurs in overweight diabetics. It is very painful, and it is difficult to walk. It is nearly always associated with swelling because the excess tissue fluid allows bacteria can proliferate. Poorly controlled diabetes with high blood sugars contribute to this problem, and poor circulation makes treatment more difficult. This can result in limb loss.
- Vein disease (Chronic venous insufficiency): Vein disease leads to aching legs, low stamina, reduced activity and weight gain which worsens the diabetes. This type of circulation problem results in stagnant poorly flowing blood and can lead to open sores on the foot or calf with uncontrolled infection and loss of the leg. The telltale sign to look for: skin discoloration in the lower calf and ankle which indicates a higher risk of skin sores developing.
Types of Diabetes
Before delving into the link between diabetes and vein health, it’s important to define the various types of diabetes and how common each classification is:
- Type 1: (represents between 5-10% of diabetics): Formerly known as juvenile diabetes, Type 1 diabetes is considered an autoimmune disorder. If you have Type 1 diabetes, your own immune system is destroying insulin producing beta cells. The end result means your body is unable to produce necessary insulin.
- Type 2: (represents 90-95% of all diabetics): This is by far the most common type of diabetes. It occurs when your cell’s resist insulin and/or your body doesn’t produce enough insulin.
- Gestational: (represents 4% of pregnant women): This type of diabetes occurs during pregnancy. It can occur in women who have never experienced diabetes before. If you have experienced gestational diabetes during a pregnancy, you have a 20-50% chance of developing Type 2 diabetes within five to ten years’ time.
- Prediabetes: (41 million Americans): If you have prediabetes this means you are not yet considered diabetic but are experiencing higher than normal glucose levels.
The Link Between Vein Health & Diabetes
- Diabetes Doesn’t Cause Vein Disease: Although studies do prove both conditions have great impact on your health, it has not been shown that diabetes causes vein disease or vice versa.
- Both cause circulation symptoms which appear similar:
- Numbness and tingling of the feet
- Skin sores in the calves and feet
- Slow circulation causing reduced stamina
- Poor circulation causing pain in the legs
- Both often have swelling present
- Both are prone to cellulitis
- They are not linked but, have common risk factors - Each of the following risk factors are applicable for both poor vein health and the onset of diabetes:
- Age
- Obesity
- Pregnancy
- Genetic predisposition
Treatment Options
- Arterial disease (PAD): Treatments focus on either opening up blockages or bypassing the blockages. This includes less invasive balloon angioplasty, laser plaque busters, stents, or roto-rooter type procedures to clean out the arteries. Less common but also effective is leg bypass surgery.
- Foot sores and neuropathy: A foot sore is often infected, so antibiotics are used and usually some surgical procedure is needed to remove the infected tissue. Non-weight bearing for weeks to months is critical to allow it to heal. Optimal blood sugar control will help healing.
- Cellulitis: The key treatment is antibiotics to fight the infection, close monitoring and adjustment to lower blood sugar and leg elevation to help with swelling. As the pain subsides with treatment, compression will help with swelling but is not tolerated in the early treatment phase due to pain.
- Vein disease (Chronic venous insufficiency): If it has progressed to result in reduced activity, weight gain or skin sores, definitive vein treatments can help and are safe for diabetics. This includes vein closure, vein removal, and injection treatments (sclerotherapy).
Prevention Methods
- Arterial disease (PAD): Stop smoking and nicotine – even one cigarette per day can constrict your arteries. Start daily walking to improve circulation and increase natural bypass blood vessels. Walk in the flat until the pain starts and keep going a few minutes, then rest and go again. If you stop for several weeks due to weather the bypass channels go away and it can be more difficult the get them back, so be consistent!
- Foot sores and neuropathy: Best prevention: daily foot exams, good fitting shoes, padding of the toes, regular visits to a podiatrist and baby every foot sore. It helps to have someone else looking at your feet daily as well.
- Cellulitis: Good blood sugar control reduces risk of infection. Getting to a lower weight will reduce pressure on your veins and reduce swelling. Wearing compression stockings, periodic leg elevation and use of a lymphedema pump can reduce swelling.
- Vein disease (Chronic venous insufficiency): If you have skin discoloration and risk for skin ulcers, wearing knee high compression stockings will reduce the risk of a skin sore developing. While lymphedema is usually not present, use of a lymphedema pump will help if swelling is significant and not controlled by stockings. These need to be used daily to be effective. A free vein screen is an easy way to sort out if treatments will help.
If you are living with diabetes, your circulation is at risk of compromise. Preventive measures can help and should be pursued if you seek to have a healthy active lifestyle. The most important goals should be healthy diet, ideal body weight, regular exercise and daily care of your feet.